Michael J. Potter, MD, FRCSC
Visiting Professor, Dept. of Ophthalmology & Visual Sciences
Biography
Associations
UBC Program in Neuroscience
Research
Research Description
Age-related macular degeneration (AMD) is the principal focus of Dr. Potter’s research program. Over the past ten years, Dr. Potter has been involved in multicenter, randomized, controlled clinical trials of new medicines for retinal diseases. He has served as a PI on several clinical studies of verteporfin photodynamic therapy for choroidal neovascularization in AMD, including the TAP study, and the VIP, VIM, VER and VIO trials. He has also participated as a PI in the Anecortave Acetate and Posurdex trials for the treatment of AMD, branch retinal vein occlusion, and central retinal vein occlusion.
Currently Dr. Potter is the Principal Investigator of a randomized, controlled, double-masked Phase II pilot study of verteporfin photodynamic therapy (at a low or very low light fluence rate) combined with bevacizumab (Avastin) for the treatment of AMD. Other studies underway include an investigation of complement gene variants and the risk of AMD in an Asian population, funded by a grant from the CNIB; a study of the role of anti-retinal antibodies in AMD; and analyses of the clinical outcomes following the treatment of wet AMD with intravitreal bevacizumab.
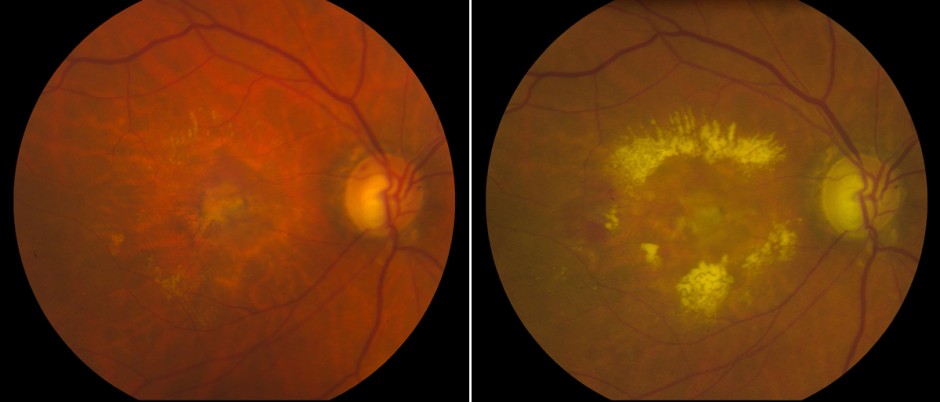
Other areas of special interest:
- Diabetic retinopathy – Combined clinical evaluations of retinal photography and laboratory testing of red cell disaggregation in diabetes mellitus
- Macular function – Electrophysiologic and psychophysical testing to evaluate macular diseases
- Developing teaching resources for ophthalmology/telemedicine on the internet
- Melanoma-associated retinopathy – Collaboration with immunologist, Grazyna Adamus, PhD, Oregon Health Sciences University
- Proliferative vitreoretinopathy – Developing a laboratory model and trial of viral inhibitors
- A laboratory model of inherited eye disease using phototransduction cascade inhibitors
- Anti-angiogenic and steroidal therapies for choroidal neovascularization in age-related macular degeneration
- Clinical outcomes following photodynamic therapy
- Idiopathic juxtafoveolar retinal telangiectasis